Acoustic Neuroma
A gamma knife case study: Acoustic Neuroma
Radiation Oncology 2011
Patient Presentation
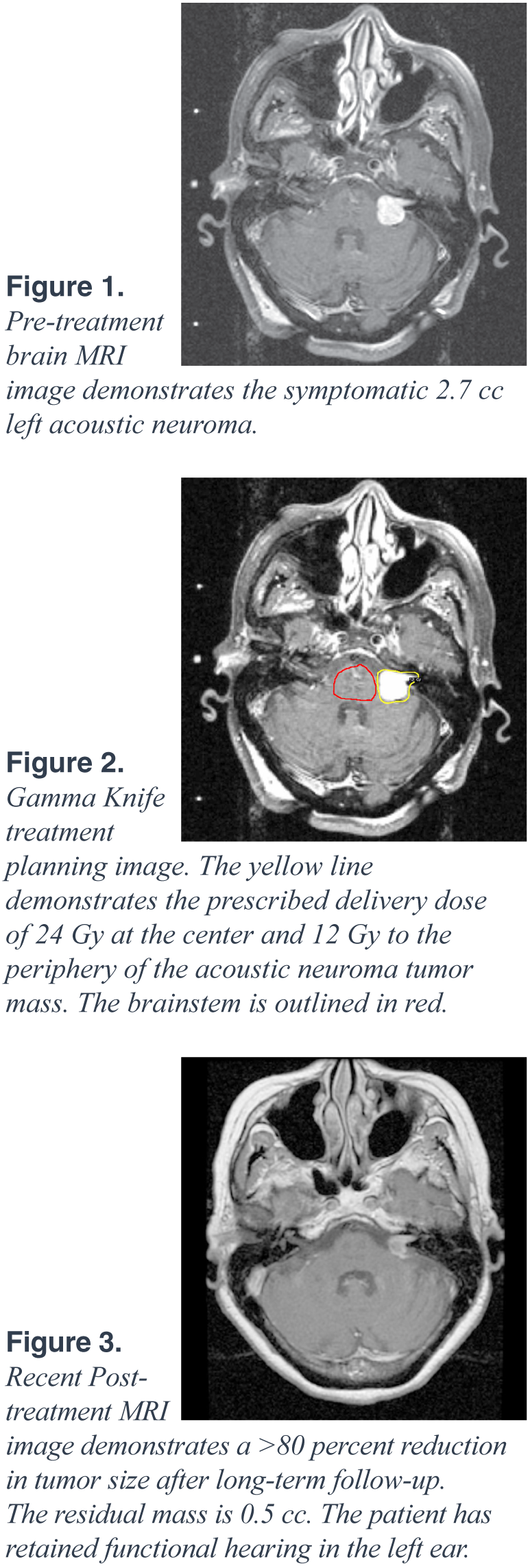
The patient is a 75-year-old female who presented to Neurosurgeon Dr. Asher Taban, MD, and Radiation Oncologist Afshin Safa, MD, with a five-year history of left-sided tinnitus and progressive sensorineural hearing loss. An MRI of the brain was performed, which revealed a 2.7 cc left-sided enhancing mass compressing the brainstem and extending from the left internal auditory canal into the cerebellopontine angle region. The radiographic features of this mass were consistent with an acoustic neuroma, which is a common benign tumor of the eighth cranial nerve. Her case was presented to our multidisciplinary Gamma Knife Review Board. Given the tumor’s size, location, and the associated symptoms of hearing loss and tinnitus, the patient underwent Gamma Knife Stereotactic Radiosurgery at Northridge Hospital Medical Center.
Procedure
On the day of treatment at the Gamma Knife Center, a stereotactic head frame was fitted and a treatment planning MRI was obtained. A three-dimensional treatment plan was developed on the Gamma Knife treatment planning workstation to deliver an ablative dose of 24 Gy at the center and 12 Gy to the periphery of the tumor, while sparing the adjacent brainstem. The radiation dose was delivered using 15 discrete spherical shots to sculpt the dose to conform to the acoustic neuroma and avoid the adjacent normal structures. The Radiosurgery treatment was delivered in less than one hour. The patient tolerated the procedure well and was able to return to normal activities later that day.
Follow-up
We have continued to follow the patient on a semiannual basis since her Gamma Knife Stereotactic Radiosurgery. She has had improvement of her tinnitus and has retained functional hearing in the left ear. Three-years after treatment, her most recent MRI revealed a 0.5 cc residual mass with necrotic center, which represents a greater than 80 percent reduction in size, as well as diminished radiographic enhancement. The patient maintains her active life and is a world traveler. She will continue to be followed by our Gamma Knife treatment team on a semiannual basis.
|
 |
|

